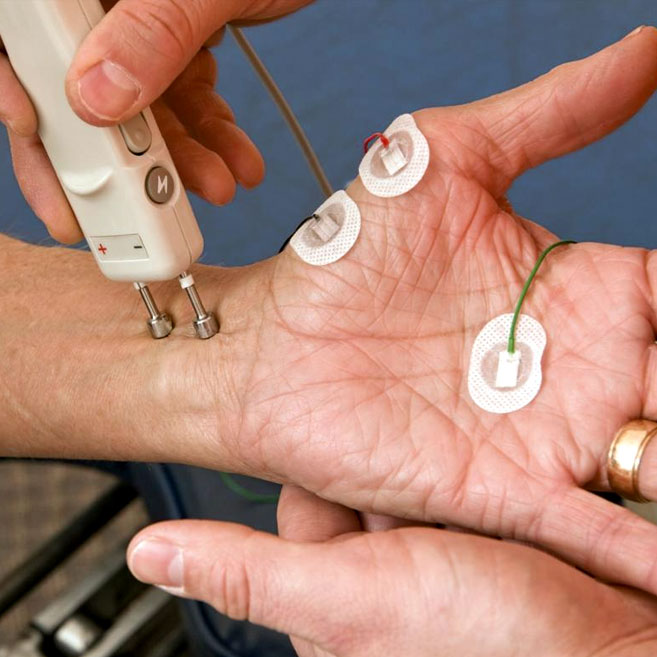
The function of the neuromuscular systems depends upon transient electrical signals emerging from nerve cells and highly localized synaptic sites and the interactivity of nerve - muscle connections and control mechanisms.
Neuromuscular Electrodiagnostic services measure the function of nerves and muscles from an electrical standpoint. These studies are an integrated discipline of Physiatry.
Studies done by Dr. Massumi are EMG, NCS and SSEP (electromyography, nerve conduction studies and somatosensory evoked potentials) - collectively known as EDX studies. These investigations – using computer -based instrumentation - help diagnose and assess nerve and muscle disorders which contribute to pain, numbness, weakness and other physical complaints and disabilities.
EDX studies serve as an extension of the clinical exam and are useful in improving the accuracy of diagnosis and prognosis.
Please see our ‘Contact’ page to call or e-mail us; You may also e-mail
info@massumi.com or call
410-825-5905.